Written by Frank M. Andrews, DVM, MS, Diplomate ACVIM
LVMA Equine Committee Professor and Director
Equine Health Studies Program
Department of Veterinary Clinical Sciences
School of Veterinary Medicine
Louisiana State University
Baton Rouge, LA
Email: fandrews@vetmed.lsu.edu
Original Publish Date June 2015Equine Cushing's Disease (ECD), also known as Pituitary Pars Intermedia Dysfunction (PPID), is a disorder that likely affects more than half the population of horses aged 15 years and older. If unmanaged, affected horses are at risk for founder (laminitis), insulin resistance (Type 2 diabetes) and because of immune-suppression, are at an increased risk of numerous infections, like sinus infections, tooth root abscesses and pneumonia.
ECD is caused by an excessive secretion of hormones from a tumor in the pituitary gland at the base of the brain. In a normal horse, the pituitary gland secretes a low level of hormones that are controlled by dopamine. As some horses age the dopamine levels decrease and the gland secretes excessive amounts of hormones like adrenocorticotrophic hormone (ACTH), аlpha-melanocyte stimulating hormone (MSH), Cortotropin-like-intermediate peptide, and beta-endorphin. These hormones cause the clinical signs (see below) that are often seen in horses with ECD.
RISK FACTORS
The primary, predisposing factor for acquiring ECD is age. Dopamine levels seem to decrease as horses get older. A recent study, found that 56% of horses 13 years or older were affected and is quite common in horses 18 years and older. Although rare in horses younger than 10 years of age, horses as young as 7 years have been diagnosed with ECD. The condition appears to be more common in pony and Morgan breeds, in horses being fed high concentrate rations and inactive obese horses and especially ponies in their younger years. Also, a potential role of oxidative stress in dopamine nerves in the brain of ECD-affected horses has been reported. Recently published information suggests that although oxidative loss of some dopamine nerves is probably normal with age, it is significantly more severe in ECD-affected horses and ponies.
MAKING THE DIAGNOSIS
In absence of a definitive, universally accepted test, diagnosis is based on history, clinical signs, and/or tests that rule out some diseases and suggest ECD.
History:
The development of infectious diseases that might not typically be seen in older horses such as chronic respiratory infections, recurring dermatitis, and dental abscesses are features of ECD. Also noteworthy is laminitis or founder in absence of an initiating event (exposure to lush pastures, grain overload, spending a lot of time on pavement). A 1993 study found that 24% of ECD-affected horses were laminitic.
Clinical signs
The telltale long shaggy haircoat is one of the most obvious suggestions of ECD. As a result of this heavy coat, many horses will sweat excessively, making them more prone to skin infections and rain rot. A pot-bellied appearance with or without a loss of muscle mass over the croup and rump. Owners often report their horses have been losing weight but it's not always a true weight loss, just a redistribution of muscle mass that makes them look skinnier on the topline. Some horses also have an enlargement of the fat pads above their eye, giving them a bulgy-eyed look.
Diagnostic Testing:
Routine bloodwork can reveal a stress response, increased blood sugar, and increased liver enzymes. In addition, a long, wooly haircoat (Wooly Mammoth [Figure 1] and founder with no apparent cause are clues that your horse may have ECD. In horses with very subtle clinical signs like, lethargy, weight loss, increased water intake, sinus infections or tooth root abscesses without changes in hair coat, might be tested by your veterinarian.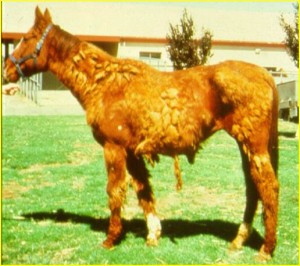
TREATMENT
ECD has no cure, but medication and management can relieve the clinical signs and side effects related to this disease. Recently, pergolide mesylate (Prascend®, Boehringer Ingelheim Vetmedica, St. Joseph, MO) was approved by the FDA for treatment of horses with clinical signs of ECD. The agent consists of a 1 mg pill given orally once daily. Pergolide is a dopamine replacement agent, used to treat Parkinsonism in people. Studies show 70% efficacy for treatment of ECD in horses. The Prascend® tablets are scored and dissolve easily in tap water. The most common side effect seen during the trial included transient loss of appetite, which went away when the drug was remove for a couple of days and horse restarted at a lower dose. A recent study showed that horses lived an average of 5.5 years after treatment owners were satisfied with treatment and according to a survey of horse owners 99% of them would treat another horse if it were diagnosed with ECD.
Besides drug therapy, management changes and supportive treatments that address side effects of ECD are important for helping to keep the horse healthy. Due to the horse's reduced immune response, maintain vaccination and deworming programs and treat infections quickly and aggressively.
Because sugar and starch can exacerbate diabetes and increase laminitis risk, limit sugar and starch intake. I recommend that owners avoid treats, apples, and especially sweet feeds -- anything that is high in soluble sugars. If you have to feed a grain, choose whole oats or crimped oats, something that is relatively high in fiber and low in soluble sugars. Testing for IR can be helpful to determine if dietary management is needed. If needed the hay can be tested for the presence of sugars and sugar content of less than 10% is ideal. If sugar content is greater than 10% then hay should be soaked in water for 30 minutes prior to feeding to reduce the amount of sugars.
Limit pasture grazing, as well, especially early in the year when the pastures have a high sugar content and the mornings after a hard, overnight freeze in late fall, when the sugar content in cool season grasses such as orchard grass, timothy, and fescues have the highest concentration of soluble sugar (up to 35%). Because some dead or dormant grass and weeds have increased amounts of carbohydrate, which can trigger laminitis in susceptible horses, they should be avoided.
We also recommend supplementing with chromium to improve insulin effectiveness and vitamin E, vitamin C, and zinc to improve immune function. However, these supplements have not been proven to be helpful for PIPD, but probably are not harmful.